Low blood sugar symptoms can appear suddenly and affect daily functioning. Drops in blood glucose levels may cause dizziness, weakness, irritability, or confusion. Individuals with diabetes, certain medications, or inconsistent eating habits are especially vulnerable, but hypoglycemia can occur in anyone. Early recognition of fatigue, trembling, or intense hunger is key to quick treatment, which can prevent serious outcomes like fainting or seizures. Maintaining a balanced diet, regular monitoring, and healthy routines helps keep blood sugar stable and ensures energy levels remain consistent. Understanding these symptoms empowers people to act fast, protecting both short-term safety and long-term health.
What is Low Blood Sugar?
Low blood sugar, medically known as hypoglycemia, occurs when blood glucose levels fall below the normal range, usually under 70 mg/dL. Glucose is the body’s main energy source, especially for the brain. When levels drop, the brain struggles to function, causing symptoms like confusion, dizziness, and poor decision-making.
The body has built-in mechanisms to restore glucose. The liver releases stored sugar, and hormones like adrenaline send warning signals. If these mechanisms fail, hypoglycemia can escalate into a medical emergency, causing seizures, loss of consciousness, or long-term health issues. Understanding low blood sugar symptoms and how your body reacts is essential for prevention and timely treatment. Awareness allows you to act immediately and maintain overall health.
Causes of Low Blood Sugar
Several factors can lead to hypoglycemia. Skipping meals or fasting is one of the most common causes. Without regular food intake, glucose levels drop, leaving the body without energy. People who skip breakfast, eat irregularly, or fast for long periods are particularly susceptible to sudden blood sugar drops.
For people with diabetes, improper use of insulin or oral medications can trigger hypoglycemia. Taking a higher dose than necessary or delaying meals can cause significant drops. Alcohol consumption also affects blood sugar. Excessive drinking prevents the liver from releasing stored glucose, increasing risk.
Other causes include illness, liver or kidney disorders, and rare hormonal or metabolic conditions. Understanding these triggers helps prevent hypoglycemia and allows people to take proactive steps to maintain stable blood sugar levels.
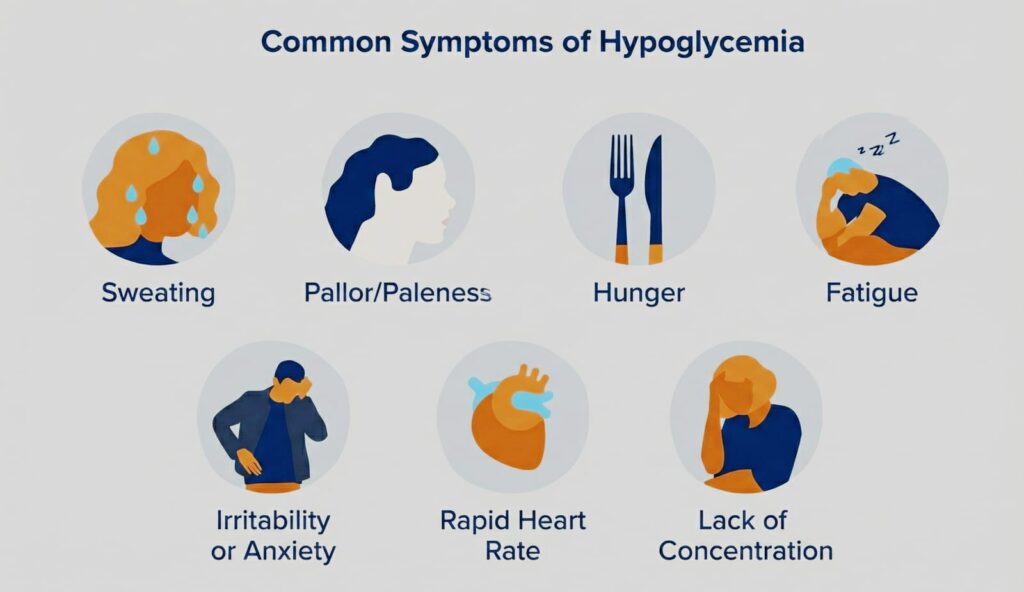
Common Symptoms of Low Blood Sugar
Low blood sugar symptoms vary in severity. Early, mild symptoms often include shakiness, sweating, hunger, fatigue, anxiety, and irritability. These signs are the body’s first warning signals and indicate the need for immediate action.
Moderate hypoglycemia affects cognitive function. Symptoms include confusion, blurred vision, difficulty concentrating, mood swings, and slurred speech. These occur when glucose deprivation begins to impact brain activity.
Severe hypoglycemia is a medical emergency. It can cause seizures, unconsciousness, or coma if not treated promptly. Recognizing the stages of hypoglycemia is critical for preventing life-threatening complications.
Symptoms Table
| Severity | Symptoms |
| Mild | Shakiness, sweating, hunger, fatigue, anxiety |
| Moderate | Confusion, irritability, blurred vision, trouble concentrating |
| Severe | Seizures, loss of consciousness, coma |
Case Study:
A 45-year-old man with diabetes noticed afternoon fatigue and irritability. Blood sugar tests showed levels dropping to 60 mg/dL. By consuming a small snack with complex carbs and protein, he stabilized his glucose and avoided severe episodes.
How Low Blood Sugar Affects the Body
Hypoglycemia affects multiple organs, primarily the brain. The brain depends almost entirely on blood glucose levels for energy. Low sugar can cause dizziness, poor judgment, irritability, and confusion. Extended periods of low glucose can impair cognitive function and memory.
The heart and nervous system are also affected. Sudden drops can trigger palpitations, sweating, and fainting. Repeated hypoglycemia may weaken these systems over time. Early recognition and treatment of low blood sugar symptoms prevent severe consequences and maintain long-term organ health.
Risk Factors
Certain individuals are more prone to hypoglycemia. Older adults, people who skip meals, and those with irregular routines are at higher risk. People with diabetes, liver disease, kidney disorders, or hormonal imbalances are particularly vulnerable.
Medications like insulin or sulfonylureas can increase risk if not properly managed. Lifestyle factors, including intense physical activity, poor sleep, and high stress, can further destabilize blood glucose levels. Awareness of these risk factors is crucial for prevention and safe management.
Diagnosis and Monitoring
Diagnosing low blood sugar requires checking blood glucose levels. Finger-prick tests provide quick results, while continuous glucose monitors offer real-time tracking and alerts.
Keeping a log of meals, physical activity, and glucose readings helps identify triggers. By recognizing patterns, individuals can adjust diet, medication, and lifestyle to maintain steady blood sugar levels. Regular monitoring is essential for people prone to hypoglycemia, especially those with diabetes.
Fact: According to the American Diabetes Association, consistent glucose monitoring reduces the frequency of severe hypoglycemic events by up to 50%.
Treatment and First Aid
Immediate treatment is critical for hypoglycemia. For mild cases, fast-acting carbohydrates like fruit juice, glucose tablets, or candy quickly raise blood sugar. Moderate hypoglycemia benefits from combining carbs with protein or fat to stabilize glucose.
Severe hypoglycemia is a medical emergency. Glucagon injections can restore blood sugar rapidly. Family members or coworkers should be educated on recognizing low blood sugar symptoms and responding promptly. Quick action prevents severe complications.
Quick Treatment Table
| Situation | Action |
| Mild | Consume 15g fast-acting sugar (juice, candy) |
| Moderate | Eat sugar plus protein/fat snack (milk, nuts) |
| Severe | Call emergency services, administer glucagon injection |
Quote: “Early recognition of hypoglycemia is lifesaving. Always keep a quick source of sugar nearby.” – Dr. Sarah Mitchell, Endocrinologist
Preventing Low Blood Sugar
Prevention relies on regular meals, balanced nutrition, and healthy lifestyle habits. Eating small, frequent meals with complex carbohydrates, protein, and fiber stabilizes blood glucose levels. Avoid skipping meals or fasting for extended periods.
Lifestyle factors are equally important. Exercise, hydration, stress management, and adequate sleep help prevent glucose fluctuations. Planning snacks before physical activity and educating family or coworkers about low blood sugar symptoms ensures rapid intervention if an episode occurs.
Lifestyle Tips and Case Studies
Real-life examples highlight prevention. A 40-year-old woman experienced afternoon crashes. Adding balanced snacks and monitoring glucose reduced episodes, improving energy. A 55-year-old man with diabetes adjusted insulin timing and walked after meals. This stabilized blood sugar levels and improved focus.
Lifestyle strategies include meal planning, light post-meal activity, hydration, stress control, and adequate sleep. Consistent small changes reduce hypoglycemia risk and improve quality of life.
Fact: Studies show that structured lifestyle changes reduce hypoglycemic events by 30–40% in people with diabetes.
FAQs About Low Blood Sugar Symptoms
What is considered low blood sugar?
Hypoglycemia occurs when blood glucose levels drop below 70 mg/dL. Individual thresholds may vary based on age and health.
What are the first signs of hypoglycemia?
Shakiness, sweating, hunger, fatigue, and anxiety are common early signs.
Can non-diabetic people experience low blood sugar?
Yes. Skipping meals, fasting, excessive exercise, or alcohol can cause hypoglycemia in healthy individuals.
How can I prevent low blood sugar?
Eat balanced meals, monitor glucose if at risk, maintain regular activity, and keep quick sugar sources available.
When should I seek emergency care?
Severe symptoms like seizures, confusion, or unconsciousness require immediate medical attention and possibly a glucagon injection.
Tips to Manage and Prevent Low Blood Sugar Symptoms
Managing low blood sugar symptoms requires awareness, planning, and consistent habits. One of the most important steps is to monitor your blood glucose levels regularly. This helps detect sudden drops early and prevents severe hypoglycemia. Eating frequent, balanced meals with complex carbohydrates, protein, and fiber keeps blood sugar levels steady throughout the day. Avoid skipping meals or going long hours without food.
Always keep quick sugars handy, such as glucose tablets, fruit juice, or candy, to treat mild hypoglycemia immediately. Planning snacks before physical activity is also crucial, as exercise can lower blood sugar. Alcohol should be consumed cautiously because it interferes with the liver’s glucose release.
Managing stress and getting adequate sleep helps maintain stable blood glucose levels, while proper hydration supports metabolism and energy. Learning to recognize early symptoms like shakiness, sweating, fatigue, and hunger allows timely corrective action. Educate family, friends, or coworkers on these symptoms so they can help during emergencies. Lastly, work with your doctor to adjust medications safely, ensuring they don’t trigger hypoglycemia.
Tips Table for Managing Low Blood Sugar Symptoms
| Action | Benefit | Caution / Notes |
| Monitor blood glucose levels regularly | Detect drops early and prevent severe hypoglycemia | Use a glucometer or continuous glucose monitor; track patterns |
| Eat frequent, balanced meals with complex carbs and protein | Maintains steady energy throughout the day | Avoid skipping meals; balance portions to prevent spikes |
| Keep quick sugars handy (juice, candy, glucose tablets) | Provides immediate relief from mild hypoglycemia | Only for emergency use; follow up with a balanced snack |
| Plan snacks before physical activity | Prevents exercise-induced low blood sugar | Choose protein-carb combination for sustained energy |
| Limit alcohol intake | Reduces risk of impaired liver glucose release | Never drink on an empty stomach; monitor sugar after alcohol |
| Manage stress and sleep | Supports stable blood glucose levels | Practice relaxation techniques; ensure 7–8 hours of sleep |
| Recognize early symptoms (shakiness, sweating, fatigue, hunger) | Allows timely corrective action | Educate yourself and those around you |
| Educate family and friends | Ensures help is available in emergencies | Teach them how to use quick sugar or glucagon injection |
| Adjust medications with a doctor | Prevents medication-induced hypoglycemia | Never change insulin or other drugs without medical guidance |
| Stay hydrated | Supports overall metabolism and energy | Drink water consistently; avoid excessive sugary drinks |
Lifestyle Tips and Case Studies
Managing low blood sugar symptoms isn’t only about medications or snacks; lifestyle habits play a huge role in keeping your blood glucose levels stable. Simple daily routines, like eating small, balanced meals, staying hydrated, and avoiding long gaps between meals, can make a big difference. Incorporating complex carbohydrates, protein, and fiber into every meal helps prevent sudden sugar drops. Light physical activity, such as walking after meals, can improve energy levels and support overall glucose control without triggering hypoglycemia.
Stress management and sufficient sleep are also crucial. High stress or poor sleep can destabilize blood sugar, increasing the risk of hypoglycemia. Mindfulness exercises, yoga, or even short relaxation breaks during the day can help maintain stable energy. Tracking your blood sugar regularly allows you to identify patterns and make small adjustments in meals, activity, or medication timing.
Case Study 1: Afternoon Crashes
A 42-year-old woman experienced sudden fatigue and irritability every afternoon. She tracked her blood glucose levels and noticed drops around 3–4 PM. By adding a balanced snack with protein and complex carbs at 2:30 PM, her energy improved, and hypoglycemic episodes reduced significantly.
Case Study 2: Exercise-Induced Hypoglycemia

A 55-year-old man with diabetes experienced shakiness and sweating during evening walks. By planning a small protein-carb snack before exercise and monitoring glucose levels, he maintained stable blood sugar levels and continued his activity safely.
These real-life examples show that simple lifestyle adjustments can prevent hypoglycemia and improve overall energy. Consistency, monitoring, and planning are key to managing low blood sugar symptoms effectively.
Conclusion
Recognizing low blood sugar symptoms is critical for health and safety. Early warning signs like shakiness, sweating, hunger, or confusion allow quick corrective action before complications arise. Monitoring blood glucose levels, eating balanced meals, maintaining a consistent lifestyle, and managing stress all help stabilize energy and prevent hypoglycemia. Real-life examples show that small, consistent habits make a significant difference. Awareness, preparation, and proactive management empower anyone to control blood sugar levels, maintain steady energy, and protect long-term health.